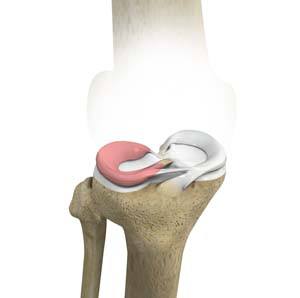
Anatomy of the Lateral Meniscus
The knee joint is formed by the union of two bones, namely the femur (thighbone) and the tibia (lower leg bone). At the junction of these two bones is a cartilage called meniscus, which acts as a shock absorber. There are two menisci – the lateral and medial menisci. The lateral meniscus is the outer meniscus of the knee joint and gives a cushioning effect during weight-bearing activities.
What is Lateral Meniscus Syndrome?
Lateral meniscus syndrome is characterized by an injury caused by the tearing of the cartilage tissue or a rare case of a congenital abnormality called a discoid meniscus, which results in knee pain.
Causes of Lateral Meniscus Syndrome
Lateral meniscus syndrome often occurs due to excessive weight-bearing and twisting motions to the knee. This occurs usually due to sports activities such as football, basketball and snow skiing, which require a lot of changes in directions and twisting movements. It can also occur due to the gradual wear and tear of tissues that occurs over time. As you grow older, degenerative changes may occur in the knee joint, causing injury with even small movements. Discoid meniscus, a congenital abnormality, is more prone to injuries while performing twisting activities.
Symptoms of Lateral Meniscus Syndrome
The common symptoms of lateral meniscus syndrome may include:
- Sharp pain associated with weight-bearing activities, twisting movements, climbing stairs, kneeling or squatting
- Audible popping or clicking of the knee on the front or back
- Swelling
- Weakness
- Locking of the knee during certain movements
- Feeling of giving way of the knee
- Tenderness
- Significant restriction of knee range-of-motion in severe cases
- Inability to straighten the knee completely
Diagnosis of Lateral Meniscus Syndrome
A thorough medical history and physical examination are performed by your doctor to diagnose lateral meniscus syndrome. Other imaging techniques, such as X-ray and magnetic resonance imaging (MRI), are ordered to confirm the diagnosis. Sometimes, arthroscopy, a procedure where a fiber-optic tube with a light and camera attached, is inserted into the knee to provide your doctor with a better view of the damage and confirm the diagnosis of lateral meniscus syndrome.
Treatment of Lateral Meniscus Syndrome
Lateral meniscus syndrome is treated with physical therapy and surgery.
- Physical therapy: This treatment includes soft tissue massage, use of crutches, electrotherapy (use of electrical energy for healing), hydrotherapy (use of water for treatment), ice or heat treatment, and progressive exercises to enhance strength, balance, and flexibility of the knee joint. Physical therapy helps to optimize the healing process and is recommended before surgery.
- Surgery: Severe meniscal injuries would require surgery, especially when you experience locking of the knee. Surgery is performed through arthroscopy, a minimally invasive surgery, by which the torn cartilage is removed or repaired.
Recovery Following Treatment of Lateral Meniscus Syndrome
If you have a minor lateral meniscus syndrome that is managed conservatively, you can return to sports activities in 2 to 4 weeks. If your condition is treated through surgery, it will take about 4 to 6 weeks for you to fully recover. Your leg will be placed in a soft bandage wrap or brace, and you may be prescribed crutches to help you walk. Surgically treated meniscus syndrome will require 6-8 weeks of physical therapy.
Related Topics
- Patellar Instability
- Multiligament Instability
- Patellofemoral Instability
- Posterolateral Instability
- Knee Arthritis
- Knee Osteoarthritis
- Knee Injury
- Knee Pain
- Anterior Knee Pain
- Meniscal Tears
- Runners Knee
- Jumpers Knee
- Unstable Knee
- Knee Sprain
- MCL Sprains
- ACL Tears
- MCL Tears
- Meniscal Injuries
- PCL Injuries
- Ligament Injuries
- Knee Fracture
- Fractures of the Tibia
- Patella Fracture
- Tibial Shaft Fracture
- Kneecap Bursitis
- Chondral or Articular Cartilage Defects
- Quadriceps Tendon Rupture
- Patellar Tendon Rupture
- Lateral Meniscus Syndrome
- Osteonecrosis of the Knee
- Knee Angular Deformities
- Osteochondral Defect of the Knee
- Articular Cartilage Injury
- Goosefoot Bursitis of the Knee
- Iliotibial Band Syndrome
- Bowed Legs
- Recurrent Patella Dislocation
- Osteochondritis Dissecans of the Knee
- Chondromalacia Patella
- Patellar Tendinitis
- Knee Sports Injuries
- Multiligament Knee Injuries
- Women and ACL Injuries
- Medial Meniscus Syndrome
- Tibial Plateau Fracture
- Tibial Eminence Fractures
- Loose Bodies in the Knee
- Osgood Schlatter Disease
- Patellar Dislocation/Patellofemoral Dislocation








