What is Patellofemoral Instability?
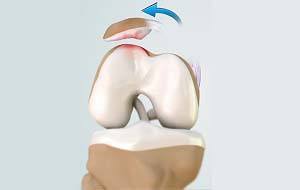
Patellofemoral instability means that the patella (kneecap) moves out of its normal pattern of alignment. This malalignment can damage the underlying soft structures such as muscles and ligaments that hold the knee in place.
Causes of Patellofemoral Instability
Patellofemoral instability can be caused because of variations in the shape of the patella or its trochlear groove as the knee bends and straightens. Normally, the patella moves up and down within the trochlear groove when the knee is bent or straightened. Patellofemoral instability occurs when the patella moves either partially (subluxation) or completely (dislocation) out of the trochlear groove.
A combination of factors can cause this abnormal tracking and include the following:
- Anatomical defect: Flat feet or fallen arches and congenital abnormalities in the shape of the patella bone can cause misalignment of the knee joint.
- Abnormal Q angle: The high Q angle (angle between the hips and knees) often results in maltracking of the patella such as in knock knees.
- Patellofemoral arthritis: Patellofemoral arthritis occurs when there is a loss of the articular cartilage on the back of the kneecap. This can eventually lead to abnormal tracking of the patella.
- Improper muscle balance: Weak quadriceps (anterior thigh muscles) can lead to abnormal tracking of the patella, causing it to subluxate or dislocate.
Young, active individuals involved in sports activities are more prone to patellofemoral instability.
Symptoms of Patellofemoral Instability
Patellofemoral instability causes pain when standing up from a sitting position and a feeling that the knee may buckle or give way. When the kneecap slips partially or completely you may have severe pain, swelling, bruising, visible deformity and loss of function of the knee. You may also have changes in sensation such as numbness or even partial paralysis below the dislocation because of pressure on the nerves and blood vessels.
Diagnosis of Patellofemoral Instability
Your doctor evaluates the source of patellofemoral instability based on your medical history and a physical examination. Other diagnostic tests such as X-rays, MRI, and CT scan may be ordered to determine the cause of your knee pain and to rule out other conditions.
Conservative Treatments for Patellofemoral Instability
If your kneecap is only partially dislocated (subluxation), your physician may recommend non-surgical treatments, such as pain medications, rest, ice, physical therapy, knee-bracing, and orthotics. If the kneecap has been completely dislocated, the kneecap may need to be repositioned back in its proper place in the groove. This process is called closed reduction.
Surgical Treatments for Patellofemoral Instability
Surgery is sometimes necessary to help return the patella to a normal tracking path when other non-surgical treatments have failed. The aim of the surgery is to realign the kneecap in the groove and decrease the Q angle.
Patellar realignment surgery is broadly classified into:
- Proximal re-alignment procedures: During this procedure, structures that limit the movements on the outside of the patella are lengthened or ligaments on the inside of the patella are shortened.
- Distal re-alignment procedures: During this procedure, the Q angle is decreased by moving the tibial tubercle towards the inner side of the knee.
The surgery is performed under sterile conditions in the operating room under spinal or general anesthesia. Your surgeon will make two or three small cuts around your knee. An arthroscope, a narrow tube with a tiny camera on the end is inserted through one of the incisions to view the knee joint. Specialized instruments are inserted into the joint through other small incisions. The camera attached to the arthroscope displays the image of the joint on the monitor. A sterile solution will be pumped into your knee to stretch the knee and provide a clear view and room for your surgeon to work. With the images from the arthroscope as a guide, your surgeon can determine any pathology or anomaly and repair it through the other incisions with various instruments.
After the evaluation is completed, a larger incision is made over the front of the knee. Depending on your condition, a lateral retinacular release may be performed. In this procedure, the tight ligaments on the outer side of the knee are released, allowing the patella to sit properly in the femoral groove.
Your surgeon may also tighten the tendons on the inside, or medial side of the knee to realign the quadriceps.
In cases where the malalignment is severe, a procedure called a tibial tubercle transfer (TTT) will be performed. In this procedure, a section of bone where the patellar tendon attaches to the tibia is removed. This bony section is then shifted and properly realigned with the patella and reattached to the tibia using screws. Once the malalignment is repaired and confirmed with arthroscopic evaluation, the incisions are closed with sutures.
Postoperative Care Following Treatment of Patellofemoral Instability
Following the surgery, your doctor will recommend pain medications to relieve pain. To help reduce the swelling, you will be instructed to elevate the leg and apply ice packs over the knee. Crutches are necessary for the first few weeks to prevent weight-bearing on the knee. A knee immobilizer may be used to stabilize the knee. You will be instructed on the activities to be avoided and exercises to be performed for a faster recovery. A rehabilitation program may be advised for a speedy recovery.
Risks and Complications Following Surgical Treatment of Patellofemoral Instability
The possible risks and complications associated with the surgery include:
- Loss of ability to extend the knee
- Recurrent dislocations or subluxations
- Arthrofibrosis (thick fibrous material around the joint)
- Persistent pain
Related Topics
- Patellar Instability
- Multiligament Instability
- Patellofemoral Instability
- Posterolateral Instability
- Knee Arthritis
- Knee Osteoarthritis
- Knee Injury
- Knee Pain
- Anterior Knee Pain
- Meniscal Tears
- Runners Knee
- Jumpers Knee
- Unstable Knee
- Knee Sprain
- MCL Sprains
- ACL Tears
- MCL Tears
- Meniscal Injuries
- PCL Injuries
- Ligament Injuries
- Knee Fracture
- Fractures of the Tibia
- Patella Fracture
- Tibial Shaft Fracture
- Kneecap Bursitis
- Chondral or Articular Cartilage Defects
- Quadriceps Tendon Rupture
- Patellar Tendon Rupture
- Lateral Meniscus Syndrome
- Osteonecrosis of the Knee
- Knee Angular Deformities
- Osteochondral Defect of the Knee
- Articular Cartilage Injury
- Goosefoot Bursitis of the Knee
- Iliotibial Band Syndrome
- Bowed Legs
- Recurrent Patella Dislocation
- Osteochondritis Dissecans of the Knee
- Chondromalacia Patella
- Patellar Tendinitis
- Knee Sports Injuries
- Multiligament Knee Injuries
- Women and ACL Injuries
- Medial Meniscus Syndrome
- Tibial Plateau Fracture
- Tibial Eminence Fractures
- Loose Bodies in the Knee
- Osgood Schlatter Disease
- Patellar Dislocation/Patellofemoral Dislocation








